The End of Our Challenge- For Now
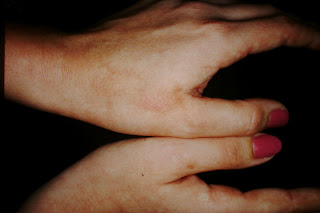
Of course, the last Q was CREST, a variant of scleroderma, and from my description there is no way you could tell whether or not it was systemic scleroderma or merely CREST, so you got credit for either answer.
Several of you wanted to know a little about me, so I will fill you in on who I am and why I chose to do the Challenge.
As most of you know, while I was in residency, I managed to amass a collection of clinical images which rivaled many of the academic programs with which I had been associated, and I always felt I needed to share them with my PAs, in a somewhat controlled way which would enhance learning and engender a desire to learn more. After casting around a bit, I hit on the idea of using wine as a reward, because it coincided with my love of wines and gastronomy in general.
After a while, we generalized it to other PAs and ARNPs, which eventually ended up with our blog getting in the neighborhood of 25,000 hits from all parts of the US and the world. Even Romania and Bulgaria! It turned out to be a lot of fun from my perspective, because I got to know some really bright, motivated people along the way, and it also honed my knowledge base a bit. I've always enjoyed general as well a surgical derm, although 90% of my practice is related to derm onc, and it forced me to remember a lot of details which otherwise would soon slip into the part of my brain devoted to baseball statistics and differential equations.
I am happily married and have a daughter Liana (seated on the couch above); her boyfriend Josh (in plaid); a son Daniel (blue shirt, who has been a subject of a couple of Q's); a daughter in law Caroline who is Quebecoise; and a marathon-running, five bar exam passing, bicycling, book writing wife with whom I spend on average an hour a night, drinking wine and talking about the world. What a family. What a life...
My hobbies are modernist cuisine, wine and bicycling, and I am currently preparing to ride all of the significant climbs of the Tour de France this July, in the Pyrenees, the Alps and Provence. I am training with Kevin Livingston, who used to be He-Who-Shall-Not-Be-Named's lieutenant on the Postal Team and Kevin now works in Austin at Mellow Johnny's, and I am lucky to have him as my coach. He's a bit of a sadist, though. He says it's for my own good. We'll see.
And, for the record, I truly believe what Lance did was no better, but no worse than any other cyclist of his era. He was just better at it, in all phases of both riding and doping, and so he became the whipping boy. And his personality is a bit strong, to put it mildly, so that also had something to do with it. It is well known that the most widely admired cyclist of all time, Eddy Merckx, used to take amphetamines prior to the mountain stages, which was a hell of a lot more dangerous than EPO and Testosterone.
So, for those of you who struggled and swore and pored over your texts (and Google), I have both admiration and a sense of kinship. You struggled, and the knowledge you walk away with is not only the specific (e.g. how to diagnose PCT) but also more important, you learned that between what you know and what you can access, there is virtually nothing you can't figure out. Your patients are very, very lucky to have you.
Lastly, BE YOUR OWN BRAND! If you do, you will always, ALWAYS have a way to make a good living, and you will be immeasurably important to those for whom you care.
Dr. B